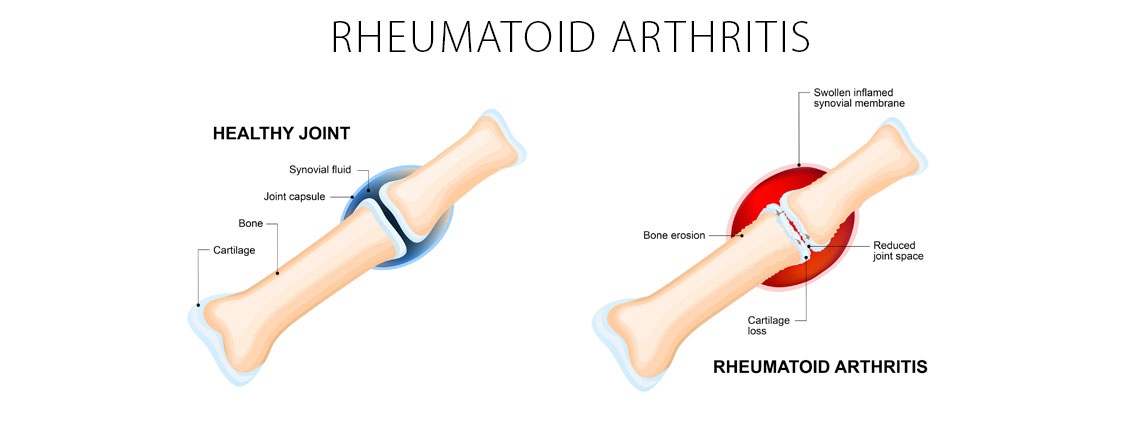
Overview
Rheumatoid arthritis (RA) is a chronic inflammatory disorder that affects mostly middle-aged adults however it can affect people of all ages. This condition is an autoimmune disorder. That means RA occurs due to your body mistakenly attacking your own tissues. If you have rheumatoid arthritis you likely experience pain and stiffness in your wrist and hand. Some patients also experience fever, loss of appetite, and fatigue. These symptoms may affect your body even when you aren’t using the joint. You might be able to feel warmth in and around the joint. Painful swelling in the wrist causes bone erosion and joint deformity.
This disease often affects the body symmetrically which means it will affect the same place on both sides of the body. As the disease progresses, it will increase in pain and the signs of deformity. You also may have rheumatoid arthritis in other parts of the body like the arms, legs, feet, or cervical spine as well. According to the Mayo Clinic, around 40% of patients report RA also affecting body systems like the skin, eyes, lungs, heart, kidney, salivary glands, nerve tissue, bone marrow, and blood vessels.
RA begins showing noticeable symptoms in smaller joints first like those that attach the fingers to the hand. Then RA will spread to other joints like wrists, elbows, and shoulders. Many patients report having flare-ups or periods of time where symptoms subside. Due to long-term inflammation of the tendons and ligaments, the joint eventually loses shape and alignment causing the deformity.
Risk Factors
Increase Your Risk
- Age. The likelihood of experiencing RA increases with age. RA is most common in those 60 years old or older.
- Sex. According to the CDC, women are two or three times more likely to develop RA than men.
- Obesity. Studies show the more overweight you are the higher your risk is of developing RA, according to the CDC.
- Smoking. Smoking cigarettes regularly increases a person’s risk of developing RA. If a person already has RA, smoking can make the symptoms worse. Smoking can make some prescription medications for RA less effective.
- Genetics. If you have a family member that has RA, you may have an increased risk. Then you can test your genes for the gene called the human leukocyte antigen (HLA) class II genotype through a blood sample. This gene indicates an increased risk of developing RA. While these genetic markers don’t confirm a patient will have RA, triggers like smoking and obesity can increase their risk.
- StressThe way your body deals with stress could worsen your symptoms. Many find that an increase in stress can cause an RA flare-up.
- Lack of Giving Birth.Women who have never given birth are at an increased risk of developing this condition.
- Life ExposureIf your mother smoked while you were a child, you’re at an increased risk. If your family was lower income when you were a child, you’re at an increased risk.
- Environmental Exposure.Asbestos and silica exposure increases a person’s risk of developing this condition. Also, those who assisted with the collapse of the World Trade Center are at an increased risk.
Recent Research
- Infections. According to research conducted by the National Institutes of Health (NIH), the following infections may contribute to RA: UTI, Epstein-Barr virus, periodontal disease, gastrointestinal infections, and infections with bacteria in the Mycoplasma genus. People who have RA are twice as likely to have periodontal disease (gum disease) than those who don’t. HIV, Parvovirus, hepatitis B and C, and alphaviruses are infections that can trigger RA.
- Gut Bacteria. According to the same study done by NIH, those with untreated RA had Prevotella copri bacteria in their intestines. Researchers indicate the bacteria found during inflammation could trigger RA. In another study conducted by NIH, scientists found balancing the microbes in the gut could prevent the RA onset.
Decrease Your Risk
- Breastfeeding. Those who have breastfed decrease their risk of developing RA.
- Healthy Diet. Maintaining a healthy diet can reduce your risk of developing RA.
Nonsurgical Treatment Options for Rheumatoid Arthritis
During an in-patient appointment, we begin by examining your hands and wrists. We will check your joints for swelling, warmth, and redness. We may suggest an X-ray to confirm the diagnosis in addition to creating a baseline. Routine X-rays will aid in tracking the procession of your condition.
Unfortunately, there’s no cure currently for RA however there are treatments available that can assist you in enjoying the activities you love. Some of those treatments are:
- Anti-inflammatory Medication. By taking an anti-inflammatory, like ibuprofen or naproxen, you can reduce the pain and inflammation associated with rheumatoid arthritis.
- DMARD Medication.. If you have RA and the other options aren’t working for you, you might try a medication called disease-modifying anti-rheumatic drug (DMARD). This drug is designed to slow the progression of RA and save your joints and tissues from permanent damage.
- Biologic Response Modifiers. This newer class of DMARDs targets the immune system that triggers inflammation which causes joint and tissue damage.
- Exercise and Therapy.. Physical therapy will help strengthen your joints.
- Splint/Brace. A splint or brace worn during activities can minimize strain on your wrist.
- Healthy Diet.Some foods like legumes, green vegetables, turmeric, ginger, seasonable fruit, and probiotic yogurt can reduce your RA inflammation. However, you should avoid animal-based products and foods high in salt and oil. Many health professionals would suggest avoiding highly processed foods, too.

